I’m currently 11 days postpartum after giving birth to my amazing and adorable daughter, Lyra. It’s unimaginable that I did not know this tiny, beautiful person just twelve days ago, and yet the experience of my natural birth plan is still fresh in my mind. My body, mind and heart permanently transformed themselves in the hours and days following her arrival, the overwhelming love, fear, protectiveness, anxiety and wonder recasting me in the tender steel of motherhood. I knew I would be giving birth to another life, of course; but what I never anticipated was that I, too, would feel reborn. Coming home after my five-day hospital stay, the space felt familiar but foreign, more like a good friend’s house than my own. As I walked through each room, I reminded myself that I was, indeed, the person who lived here. The person who bought those groceries and changed those sheets and painted her nails at that kitchen table. Yes, that was me who did all those things. But, somehow, I knew I was no longer that woman.
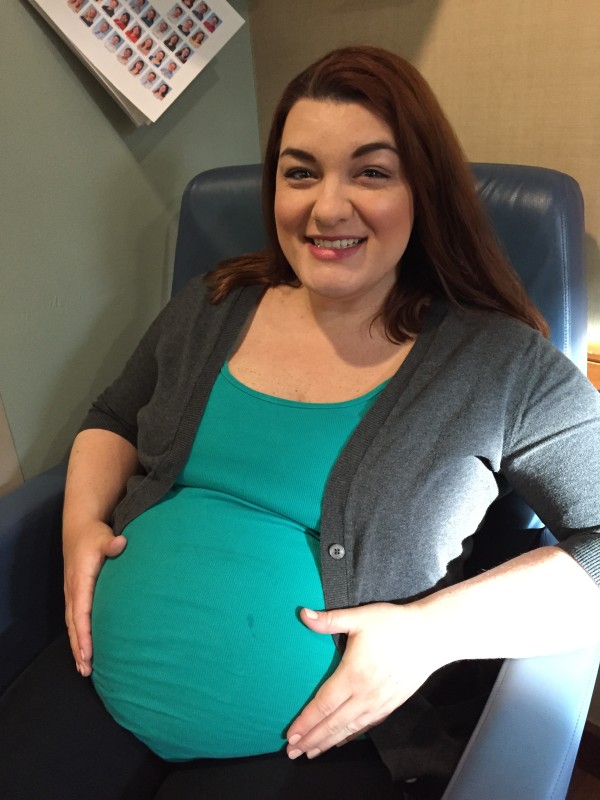 After my post detailing my plan for a drug-free childbirth, I thought I owed everyone an update on how it all went down. The plan became a bit more complicated when I was diagnosed with gestational diabetes at 28 weeks. Due to the risk of an overly large baby, my doctor told me I would need to be induced on my due date if the baby had not yet arrived. The last week of my pregnancy, I tried every natural remedy under the sun to get my labor going: evening primrose oil, raspberry leaf tea, walking, sex, nipple stimulation, spicy food, chiropractic adjustments, acupuncture. Despite my efforts, my induction date of Thursday, April 2, arrived, and my husband and I checked into Methodist Hospital downtown knowing, God willing, we’d leave as three.
After my post detailing my plan for a drug-free childbirth, I thought I owed everyone an update on how it all went down. The plan became a bit more complicated when I was diagnosed with gestational diabetes at 28 weeks. Due to the risk of an overly large baby, my doctor told me I would need to be induced on my due date if the baby had not yet arrived. The last week of my pregnancy, I tried every natural remedy under the sun to get my labor going: evening primrose oil, raspberry leaf tea, walking, sex, nipple stimulation, spicy food, chiropractic adjustments, acupuncture. Despite my efforts, my induction date of Thursday, April 2, arrived, and my husband and I checked into Methodist Hospital downtown knowing, God willing, we’d leave as three.
Based on everything I’d read about induction, the more favorable the cervix is for labor at the start of the process, the smoother it goes. My doctor had told me I was only one centimeter dilated at my 39-week appointment and not very effaced, so as the on-call doctor at Methodist checked me, I silently prayed I’d made good progress. My plan was to start with the lowest dose of Pitocin and hope it kicked me into labor; then, maybe I’d have a shot at still forgoing pain meds. He reported I’d unfortunately made no additional progress–still only one centimeter. We would have to do 12 hours of a cervical ripening drug called Cervadil before moving forward. We spent the next 12 hours watching Netflix, reading and trying to rest as the Cervadil did its work, with nurses coming in seemingly every ten minutes to readjust the fetal monitors. At the 12-hour mark, the doctor reported that I’d only progressed one additional centimeter, and we’d need to move on to another drug called Cytotec. We did two four-hour rounds that unfortunately produced little result. I became increasingly worried and frustrated at how poorly my body was responding to the induction. Clearly, the baby was not ready. Gestational diabetes already carries a 50 percent C-section rate, and being induced only raises that risk.
Around 4:30 a.m. on Friday morning, my water broke and I began having regular contractions. My husband and I spent the next few hours working through the contractions in accordance with our Bradley Method pain management plan, hopeful that my body would go into labor on its own and we could avoid Pitocin entirely. Unfortunately, the contractions decreased in strength over time, eventually petering out completely. At 10:00 a.m. on Friday, April 3, they started me on the Pitocin drip. I was still only two centimeters, far from ideal for starting Pitocin. As the nurse hooked me up to the IV, huge tears began to roll down my cheeks. I knew Pitocin causes unnaturally painful contractions that place a lot of stress on the baby. I took a minute to emotionally process the deviation from my ideal plan, and then I steeled myself for the coming storm.
And what a storm it was. My husband and I spent the next 18 hours working through increasingly torturous contractions using relaxation, massage, music and other natural techniques. I could not have asked for a better coach, and for many hours the pain was intense but bearable. By late that evening, my ability to cope had started to break down. Family members took turns sitting next to me holding my hand as horrifying back labor pain radiated through my body like lava. I had lost the ability to communicate, moaning and sobbing through each contraction. The hospital staff had cranked up the Pitocin to the maximum level. Around midnight, I was at nine centimeters, and we were hopeful the end was near.
The next three and a half hours were truly some of the darkest of my life. The contractions came right on top of each other, pain so overwhelming I struggled to stay conscious. I felt like an animal caught in a trap. The doctor came to check me and woefully informed me that I was still at nine centimeters–no progress in almost four hours. I sobbed hysterically and begged her to tell me when it would be over. She told me there was nothing to do until I progressed that last centimeter, and she couldn’t tell me why I wasn’t getting there. At this point, I turned to my husband and told him I needed a mild epidural. After almost two days in the hospital with no sleep or food and 18 hours of unimaginable pain, my body was completely broken down. I knew there was no way I’d have the energy to push a baby out in this state. After confirming that it was what I really wanted, a team of anesthesiologists arrived ten minutes later to administer the relief. Within an hour, I was 10 centimeters and ready to push. It seems the epidural had allowed my body to relax enough to dilate fully.
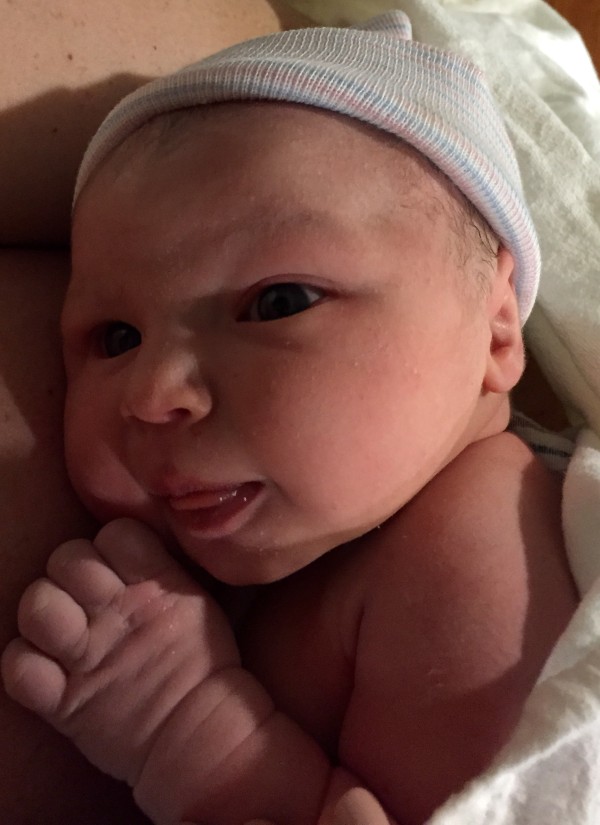 We quickly realized pushing was not going to go quickly, either. One hour passed, then two, then three. The doctor had warned me she would only allow me to push for three hours before taking me to C-section. Thankfully, I’d made enough progress at the three-hour mark that they agreed to let us continue. With the mild epidural, I was able to feel each contraction and the pressure of the baby descending, allowing me to push effectively. Finally, at 8:51 a.m. on Saturday, April 4, Lyra Jane Palmer slipped from my body and let out a glorious scream.
We quickly realized pushing was not going to go quickly, either. One hour passed, then two, then three. The doctor had warned me she would only allow me to push for three hours before taking me to C-section. Thankfully, I’d made enough progress at the three-hour mark that they agreed to let us continue. With the mild epidural, I was able to feel each contraction and the pressure of the baby descending, allowing me to push effectively. Finally, at 8:51 a.m. on Saturday, April 4, Lyra Jane Palmer slipped from my body and let out a glorious scream.
In a stunned and enthralled voice, my husband announced she was a girl and cut the cord as we stared at each other in utter wonder. She measured 20.5 inches and weighed 7 lbs 14 oz. After all the concern about her size, she ended up being absolutely perfect. She came out face up, which explained the horrific back labor I’d experienced and why it took so long to push her out.
I truly believe the light epidural was the right decision for me, and probably saved me from having a C-section. It was administered right as I was nearing the 24-hour mark of my water breaking, after which the risk of infection goes way up. And knowing now how long it would take to push her out, there’s no way I could have done it with some relief from the pain.
I don’t consider myself to have “failed” at natural birthing. If I had been allowed to go into labor naturally, I’m confident I could have gone completely drug free; those 18 hours on the Pitocin drip showed me just how strong I am. And if we are lucky enough to have a second child, I still hope to go drug free if possible. Given the circumstances of my induction and Lyra’s position in the birth canal, there’s no doubt in my mind I did my best. I labored without drugs for as long as I could, which means the baby received as little exposure to pain medication as possible. She was extremely alert at birth, scoring tens on both her APGAR tests, which the doctors said is practically unheard of. I avoided a C-section, and our breastfeeding relationship is off to a great start. I achieved every goal on my list, and I’m damn proud of what I went through to bring our perfect little girl into the world.








